Venous Leg Ulcers
Home » Venous Leg Ulcers
Causes of Venous Ulcers


Pathophysiology of Venous Ulcers

Deep Vein Thrombosis (DVT)
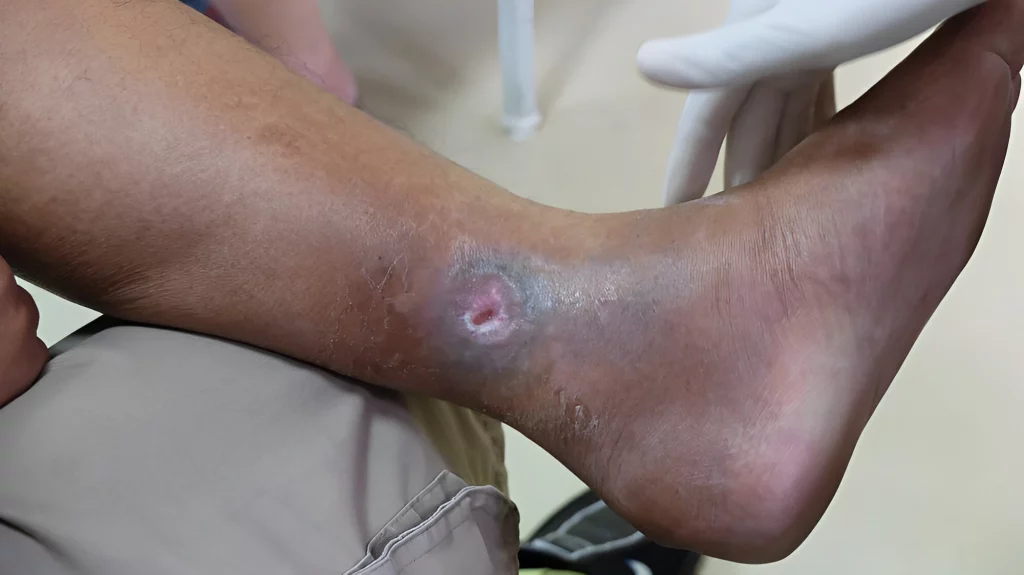
Symptoms and Treatment of Venous Ulcers
- Leg swelling, cramping, and “heaviness”
- Itchy, flaking, or thinning skin in the feet and ankles (“stasis dermatitis”)
- Shiny, tight, warm, or distended skin
- Dark red, purple, or brown skin (sign of fluid leaking into the tissue)
- Formation of a small shallow sore with irregular edges
- Keep the wound clean and bandaged
- Keep the dressing dry. Moisture can soften healing tissue, causing the wound to get bigger
- Clean and change the bandages according to instructions from your doctor
- Wear compression stockings to reduce fluid pressure in your legs
- Keep your leg elevated as much as possible
- Walk or engage in other exercises. This improves blood flow and promotes healing
Preventing Venous Ulcers


Treating Venous Ulcers
- Control the swelling
- Treat the wound by removing biofilm
- Encourage patient engagement
Control the swelling. Compression is key to dealing with venous ulcers. Many patients resist compression wraps or stockings because they are painful and difficult to apply. If patients and caregivers can find a solution that works for both of them, this is the number one key to treating ulcers, because wounds need good circulation to heal, and compression helps improve circulation.
Treat the wound by removing biofilm. Although the need to remove dead tissue (“debridement”) has always been known, there is a growing understanding that biofilm, a thin layer of biological material that attracts bacteria, must be prevented in order to promote healing. Remedium offers a full line of holistic treatments in line with current best practices to keep these wounds free of stubborn resistant biofilm in wounds.
Encourage patient engagement by involving them in their care. Patient compliance to treatment is one of the largest challenges that treating venous leg ulcers have. Older patients may not understand why they need to carry out all these wrapping and cleaning regimens, especially if the doctor doesn’t bother to explain them. Education encourages patient compliance and helps reduce potential recurrence of the ulcers.
